Together, we can positively impact patients living with alopecia areata
Alopecia areata (AA) is a chronic, complex, systemic, immune‑mediated disease characterized by sudden, non‑scarring hair loss on the scalp, face, and/or body. Beyond hair loss, patients often experience a significant psychosocial burden.
Learn more about AA and its impact below:

Disease Education
The better we understand AA, the better prepared we will all be in helping patients gain control over this disease.
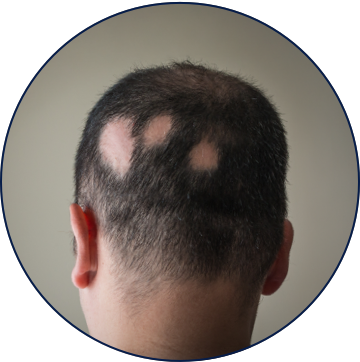
TYPES OF ALOPECIA AREATA
Common Scalp Presentations
About 14%–25% of patchy AA cases progress to alopecia totalis or alopecia universalis.2,3
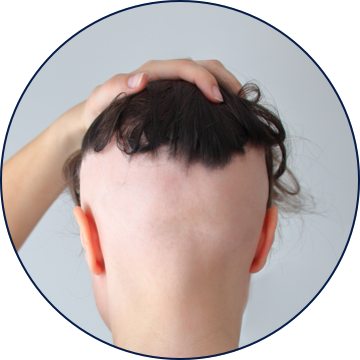
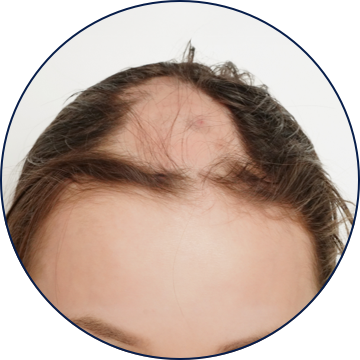
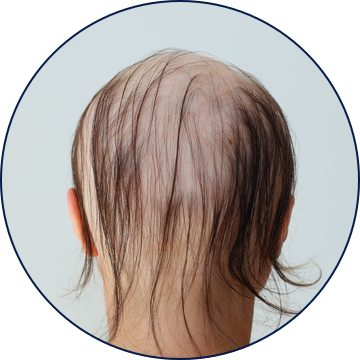
TYPES OF ALOPECIA AREATA
Uncommon Scalp Presentations
Regrowth in one region of the scalp may be associated with expanding areas of alopecia elsewhere.3
TYPES OF ALOPECIA AREATA
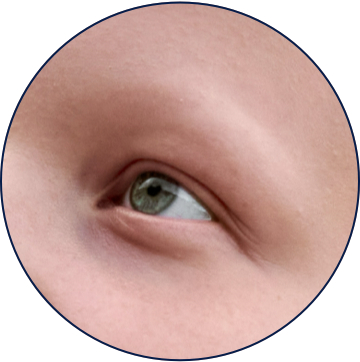
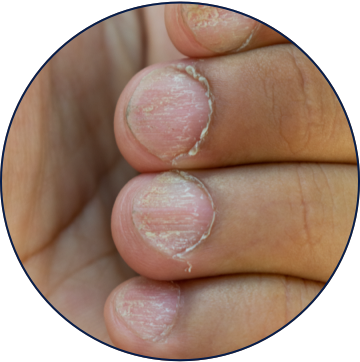
Non-Scalp Presentations
Eyebrow hair and eyelash loss can result in dryness and irritation in the eyes and an inability to keep debris or sweat from the eyes.1
THE EPIDEMIOLOGY OF ALOPECIA AREATA
Key Data and Demographics
The estimated prevalence of AA is 0.2%–2% of the population. AA affects females approximately 1.3x compared to males.1,7-9
An estimated 42% of AA patients have severe AA
as defined by the Severity of Alopecia Tool (SALT) score ≥50 and 58% have mild to moderate disease (SALT <50).7
Pediatric diagnoses represent approximately 20% of cases.10,11 Up to 40% of patients will present with their first AA patch before age 20.1,12
Non-white ethnicities have an increased risk of developing AA. Asian ethnicities have a 3x higher rate of AA compared with white ethnicities.13,14
BURDEN AND COMORBIDITIES
AA patients have a higher prevalence of immunological and psychiatric comorbidities7
The psychosocial burden in AA may be profound. Patients often face both public- and self-stigmatization.2,15-18
Up to 68% of patients with AA present with mental health symptoms. Diagnoses of anxiety and/or depression are more prevalent in AA vs age- and gender-matched controls.15,16
AA can significantly impact social and professional functioning and influence major life decisions.2,16
Increased risk of immune-mediated conditions in patients with AA vs controls without AA19
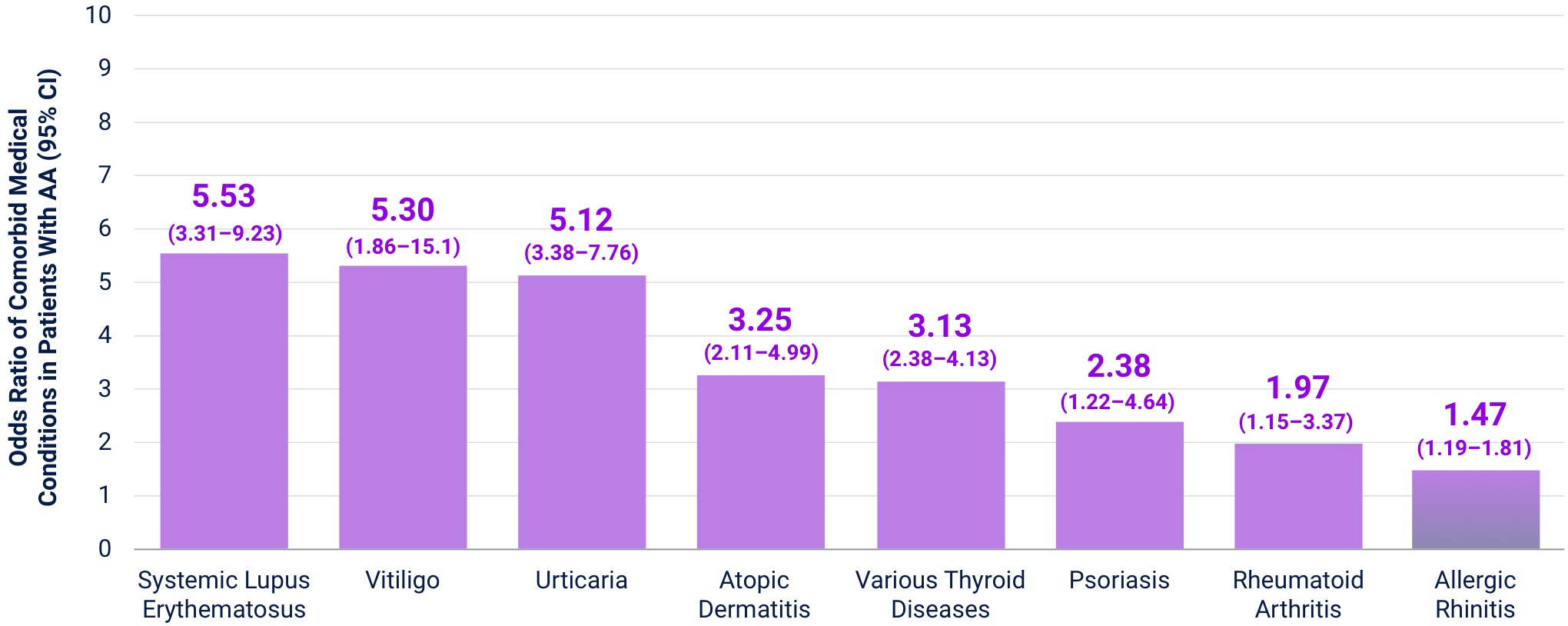
AA is associated with a 43% higher risk of new-onset atopic dermatitis (AD) and a 45% higher risk of other, new onset immune‑mediated conditions.19,20*
References: 1. Mesinkovska N et al. J Investig Dermatol Symp Proc. 2020;20(1):S62-S68. 2. Lepe K et al. Alopecia Areata. In:StatPearls;2024. 3. Pratt CH et al. Nat Rev Dis Primers. 2017;3(1):17011. 4. Lintzeri DA et al. J Dtsch Dermatol Ges. 2022;20(1):59-90. 5. Nguyen B et al. Am J Clin Dermatol. 2023;24(1):55-67. 6. Nwosu A, Miteva M. Skin Appendage Disord. 2023;9(3):179-186. 7. Benigno M et al. Clin Cos Inv Dermatol Clinical. 2020;13:259. 8. Mostaghimi A et al. JAMA Dermatol. 2023;159:411. 9. Villasante Fricke AM. Clin Cosmet Investig Dermatol. 2015;8:397. 10. Alkhalifah A et al. J Am Acad Dermatol. 2010;62(2):177-190. 11. O’Connor LF et al. Arch Dermatol Res. 2022;314(8):749-757. 12. Fricke AM. Clin Cos Inv Dermatol Clinical. 2015;8:397-403. 13. Harries M et al. Br J Dermatol. 2022;186(2):257-265. 14. Jang H et al. Eur J Clin Invest. 2023;53(6):e13958. 15. Ghanizadeh A et al. Int J Trichology. 2014;6(1):2-4. 16. Muntyanu A et al. J Eur Acad Dermatol Venereol. 2023;37:1490-1520. 17. Creadore A et al. JAMA Dermatol. 2021;157(4):392-398. 18. Kacar SD et al. Int J Trichology. 2016;8(3):135-140. 19. Ly S et al. Am J Clin Dermatol. 2023;24(6):875-893. 20. Holmes S et al. Clin Exp Dermatol. 2023;48(4):325-331.
Alopecia Areata Explained
You and your patients have many treatment options—such as topicals and systemic therapies—to consider for AA.
Take a look at information that may help with your treatment considerations.
UNDERSTANDING THE MECHANISM OF DISEASE
Watch how AA operates at a cellular level and learn what immune-mediated pathways can be targeted to help hair follicles return to a normal growth cycle.
Expert Exchange
Understanding AA and supporting patient-centric communications.

Making Each Moment Count: Meaningful Engagement With Our Patients
Goal Setting and Individualizing Targets With Our Patients
Understanding the Comprehensive Severity of AA for Patients
Helping Patients Navigate the Psychological Burden of AA
Tailoring Our Care: How Should Care Differ for Adult Patients vs Adolescents?
The Invisible Trauma of Alopecia Areata
Patient Stories
Watch these patient stories to gain a deeper understanding of how a life can be changed by AA.